Treatment of diabetes induced by a pancreatic illness
(pancreoprivic diabetes Typ 3 c) - one of the most difficult problems
The pancreas produces hormones and enzymes and is one of the largest glands in the human body. It fulfils central functions in nutrient and energy balance, together with the liver. It also regulates digestion and the blood sugar level.
If it is surgically removed (pancreatectomy) then there are no more enzymes to aid digestion (exocrine function). But, at the same time, the most important hormones which regulate the blood sugar level in the body are missing. Although insulin can be replaced subcutaneously the “opposing partner” glucagon is still missing, which is necessary to maintain the fine balance in the blood sugar levels.
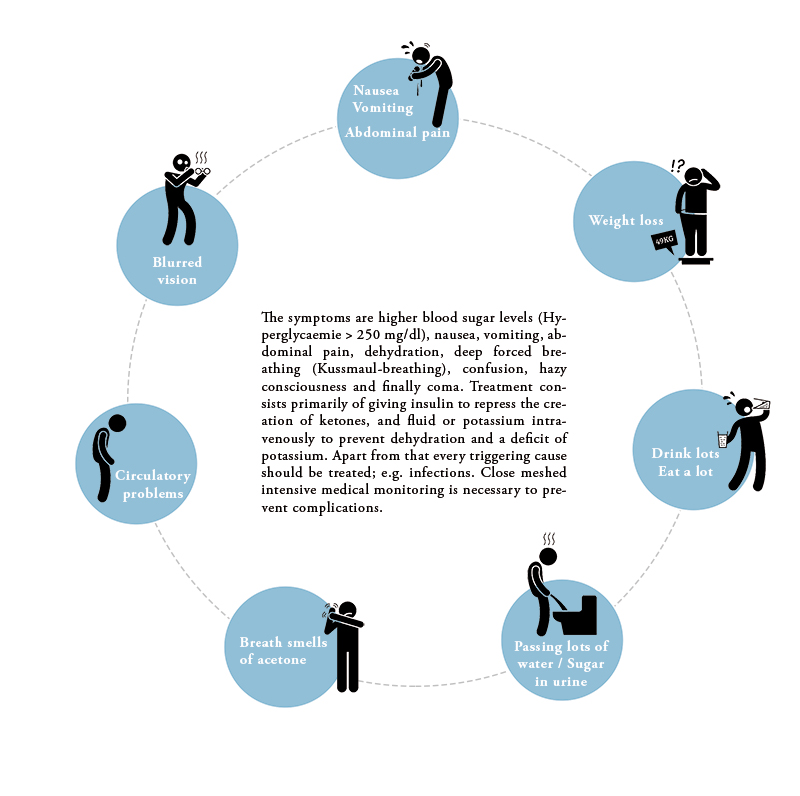
The result is an instable blood sugar level, with inestimable amounts of sugar flowing into the blood. High blood sugar peaks which increase rapidly are replaced by very low blood sugar levels verging on hypoglycaemia several times a day. There’s a high risk of low blood glucose (severe hypoglycemia) or acidosis due to fat-burning, which takes place by insulin-deficiency and/or fasting.

Blood sugar (glucose) measurement
Blood sugar measurement is the basis for a successful blood sugar control.
Blood sugar self-monitoring has to be learned. Inhibitions about pricking oneself must be overcome. It’s very important to encourage motivation to manage the day-to-day control, as a structured blood sugar management is the basis of stability.
This involves measuring the blood sugar level at certain given times with dependable blood sugar measuring technology. Documenting, saving the measuring results and interpreting the results has to be learned. Some action or other should follow as a reaction to the results. Eight blood sugar measurements in the course of the day are necessary for blood sugar control (pre-food, before meals, 1-2 hours after meals, when you go to bed and in the night).
Everyone who has undergone a pancreatectomy requires a blood sugar measuring device as well as a ketone measuring device. If the blood sugar levels are over 250mg/dl, then, a ketone measurement should be done as well as a blood sugar test.
The continuous blood sugar measurement (CGM) and the Flash Glucose measurement (FGM) make a 24-hour blood sugar measurement possible in many single measurements in a short time. And the result of this is a good overview of the measurements and therefore a better blood sugar control.
Flash Glucose Mesaurement (FGM)

This is a very practical thing for people after a pancreatectomy. It doesn’t require any blood sugar sticks and is water resistant, so that showering is not an issue. The system can be worn in the arm for up to 14 days. It offers a pain-free blood sugar measurement with a frequency of 1 measurement per second. The test gives the present blood sugar measurements and the course of the measurements over the past 8 hours as well as the blood sugar trend. FMG is a great help in the day-to-day self-management situation regarding the choice of food and the effect of movement on blood sugar.
Nutritional Recommendation
Up to 8 small meals per day are recommended. The amount of fat should be restricted in the dietary composition and foodstuffs favoured, which are high in protein. Nothing is forbidden and personal preferences can help to make sure that sufficient calories are consumed. Enzymes should be taken with each meal – rather too many than too few! It’s not necessary to calculate the amount of fat for the enzymes.
In order to allow the body to digest the meal undisturbed through fluids, no drinks should be served with the meals and also up to 30 minutes before and after meals.
Therapy goals
The maintenance of a high life quality after a pancreatectomy or even the improvement of it is the main goal. Intensive client-oriented support is necessary for that. It is important, therefore, to avoid unnecessary restrictions and to be understanding in the face of things like fatigue, loss of appetite, diarrhoea and constipation.
The medical goals are ensuring good nutrition and stable blood sugar levels while simultaneously avoiding episodes of hypoglycaemia, ketoacidosis or hyperglycaemia (Blood sugar > 250 mg/dl). The blood sugar levels should be 100-120 mg/dl before food and also before meals and the level one hour after food should be 180 mg/dl.
Diabetes Training
The most important first step is a diabetes training. After a pancreatectomy, patients need insightful diabetes coaching within the diabetes training, so that they lose their fear of the illness and also their feeling that the demands are excessive. The feeling of being in control of their diabetes has to be learned. Diabetes training helps the understanding of the illness and of the health-risks. Training strengthens the intrinsic motivation, to occupy oneself with diabetes and its self-management. During the training behavioural strategies are encouraged and practical skills taught. With this a positive attitude to the therapy goals can develop.
Needle and Injection technique
It’s important to use a different place for each injection. Changing the position once a day is not enough! The next injection should be placed 2-3cm away from the previous one. If insulin is always injected into the same part of the body, then the fatty tissue under the skin can change – it sticks together and scars. This typical change is called lipohypertrophy. Sometimes diabetic people deliberately choose such places for the injections, as this altered tissue is less sensitive to pain. However, the tissue alterations will only increase through that.
Repeated use of pen-needles also assists the development of lipohypertrophy: a re-used needle is blunter and injures the tissue more than necessary. The circulation is also changed in such tissue and an insulin injection therefore leads to fluctuating blood sugar levels and a higher need for insulin. Unexpected results of low blood sugar can then occur after an injection into healthy fatty tissue beneath the skin.
Needles with a length of 4mm, 5mm, 6mm and 8mm can be used by every adult patient, including overweight people. There is no medical reason to recommend needles with a length of more than 8mm for adults.
Insulin Pump Therapy (Continuous subcutaneous insulin infusion = CSII)
Insulin Pump Therapy is the nearest thing to physical insulin substitution. The basal rate can be individually and hourly programmed with a continuous release of fast-working synthetic insulin. A registered dietician can calculate the necessary amount of insulin required for a meal.
Different sorts of bolus insulin are available, e.g. a lengthened bolus or dual bolus. The advantages of the pump therapy are the low daily insulin requirement and low BE-factors. A finer adjustment is possible with this.
It’s simpler to correct high results. There’s proof of less occurrences of too low blood sugar.
Adjusting the insulin therapy to irregular meals, movement or infections is easier.
The disadvantages are local infections and scarring in the tissue at the point of entry of the catheter, catheter blockage or disconnection as well as the danger of ketoacidosis.
The artifical endocrine pancreas - an option for the future

Continuous insulin infusion – requirement and component of technical systems on the way to a closed loop. Further components are blood sugar measuring device to calibrate, a glucose sensor with a transmitter and a computer for diet management. A future aspect is also the dual pump with insulin and glucagon.
Hypoglycaemia
We talk of hypoglycaemia when the blood sugar level falls below 70 mg/dl (3.9 mmol/l) – regardless of the symptoms! A blood sugar level of 70 mg/dl (3.9 mmol/l) is the borderline for most people to a lack of sugar in the brain.
Low blood sugar is a condition which is characterised by a stress reaction of the body to the lack of sugar and / or signs of a lack of sugar to the brain as well as very low blood sugar measurements and an improvement in the symptoms after consuming carbohydrates. If the blood sugar level was very high previously, then the signs of low blood sugar are noticeable, even although the levels are still high.
Signs of the stress reaction to the lack of blood sugar are sweating, trembling, a racing heartbeat, hunger, state of anxiety, lack of concentration and dizziness. Confusion, aggressiveness and loss of consciousness are signs that the brain is already suffering from a lack of sugar.
A hypoglycaemia attack in the night can be established by measuring the blood sugar before food. Other symptoms are if the person has a headache or feels as if he/she got no sleep. Apart from that nightmares, a rumpled bed, soaked nightclothes and very restless sleep during the night point to a hypoglycaemia attack.
An especially bad case of hypoglycaemia is indicated when the person requires external help (e.g. through relatives or medical personnel). This type of low blood sugar constitutes a medical emergency and must be treated by a doctor. It is particularly important to find out what triggered the attack in order to prevent it happening again.
The importance of a potentially evolving hypoglycaemia perception disorder.
Repeated hypoglycaemia attacks lead to a decreasing ability for adequate perception of low blood sugar levels, which can be connected to a 9-fold rise in serious cases of hypoglycaemia. These patients can sometimes show blood sugar levels of under 2.0 mmol/l without specific symptoms. This kind of perception disorder can be evaluated with the help of patients’ self-assessments and reports (low blood sugar measurements without corresponding symptoms) or by using a particular questionnaire e.g. from the Diabetes-Akademie in Bad Mergentheim (under www.hypos.de). An adequate (but not too low) control of blood sugar levels in the long-term is key in overcoming the lack of not being able to notice when things are bad.

The basic rule when blood sugar is too low is to "eat fist measure later" as soon as you notice the first signals.
If the blood sugar level is very low before it is noticed, then there is not a lot of time to waste! You need to react quickly and you should have practised the self-treatment routine. You should always carry dextrose or some other “treatment” like Coca Cola, fluid glucose, lemonade or fruit juice with you.

After 15 minutes measure bllod sugar again.
If the results are over 120mg/dl, then the danger has past. A “hypo-box” saves time and is very useful. The dextrose is kept in a small tin – unwrapped – and you can take that everywhere with you. To treat low blood sugar levels you should take 4 pieces of dextrose and after that 2 BE which work for a longer time.
If someone loses consciousness through a hypoglycaemia, then relatives can inject glucagon intramuscularly, to treat the seriously low blood sugar level.

Glucagon nose spray
There’s a new glucagon nose spray (3 mg), which is not yet approved in Germany. This is just as effective as the injection and needs only around 10-20 minutes to take effect.
If cases of low blood sugar happen regularly – and especially if the person does not notice it himself, then specially trained dogs may help and be able to warn the person.
Ketosis
Ketones are produced in the liver as an alternative energy substrate, when there is not enough glucose left. This is a physiological process which ensures the energy supply of heart and nerve cells.
Ketosis or extreme ketogenesis can occur when the insulin level drops or there is no insulin production at all, extreme insulin resistance in cases of hunger or low carbohydrate diets. Ketosis can also occur during times of physical stress caused by infections, during long-term physical strain as well as due to alcohol consumption (suspension of gluconeogenesis). Ketoacidosis is a metabolic hyperacidity of the blood. Diabetic ketoacidosis develops when there is absolutely no insulin or so little that it leads to an increased oxidative catabolism of fat with the subsequent creation of acid ketones. Ketoacidosis only develops when there are more acidic ketones than blood and tissue can handle.
Ketoacidosis often occurs after a pancreatectomy when basal insulin is forgotten or the effect doesn’t last the full 24 hours. Ketoacidosis is an emergency situation and needs to be treated by a doctor – even in mild cases. Ketoacidosis can quickly develop to an extremely serious medical situation.