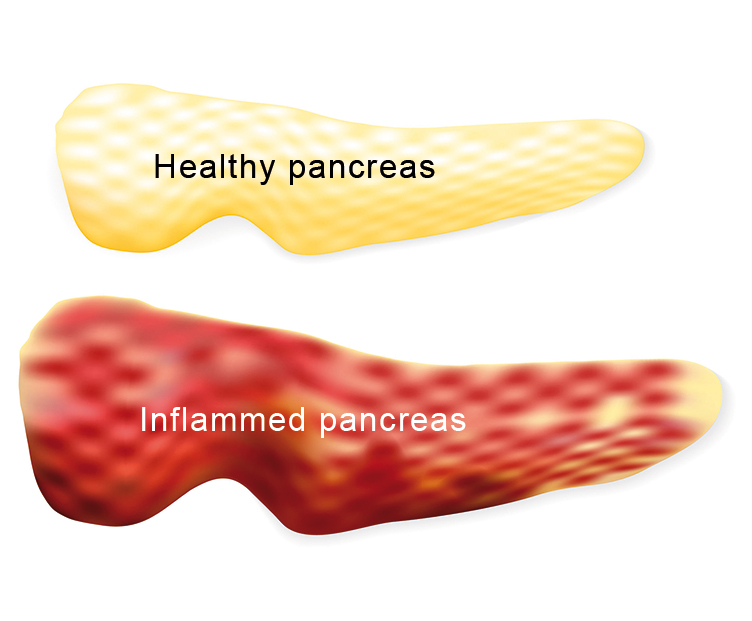
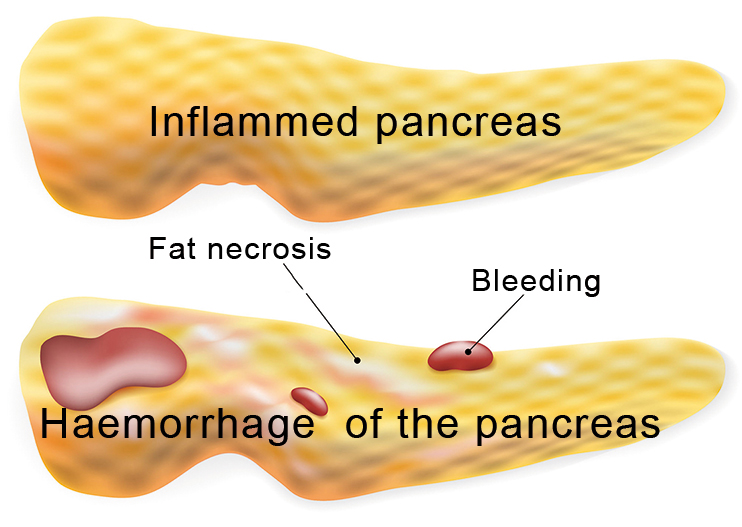
Chronic inflammation of the pancreas
Chronic Pancreatitis is an ongoing, permanent inflammation of the pancreas, which can come in bursts or run continuously. The inflammation leads to the healthy pancreas tissue gradually being replaced by scarred tissue, which eventually leads to the exocrine glands no longer functioning (digestive enzymes) and, in the end, also the endocrine glands giving up (insulin).
Alcohol abuse, smoking, blocked bile ducts and genetic or hereditary factors. In addition to that there are also the autoimmune causes (autoimmune pancreatitis and cases where the cause cannot be determined (idiopathic). When the cause is hereditary repeated bursts of acute pancreatitis appear early on, which change to a chronic calcified pancreatitis in the course of the illness. Mutations in different genes are responsible: (PRSS1, SPINK-1, CFTR, CTRC). Should the family history indicate that there is an increased risk of developing cancer, then genetic counselling and a genetic diagnosis should be conducted.
With chronic pancreatitis the individual course of the illness can vary considerably and without any fixed temporal order. The symptoms are: strong pain in the upper abdomen, radiating in a ring around the abdomen, loss of weight, fatty stools, flatulence, diarrhoea, vitamin deficiency, possibly jaundice and metabolic problems because of insulin reduction. Complications of the illness can lead to further problems and symptoms (splenic vein thrombosis, fistula, pseudo cysts, blockages of the bile duct and the pancreatic duct etc.) Chronic pancreatitis can be classified as mild, moderate or severe.
In addition to the symptoms and discomfort, the following methods can be used to assist diagnosis: ultrasound, endosonography (EUS), MRCP magnetic resonance cholangiopancreatography, computed tomography (CT) and magnetic resonance tomography (MRT) and the laboratory results (amongst others higher lipase, stool-elastase.
Significant factors for the success of the treatment are: removal of causes (e.g. abstinence from alcohol) adequate pain therapy, dietary counselling, sufficient intake of digestive enzymes and treatment of a beginning diabetes. In the course of the illness an endoscopic or an operative intervention may be necessary for some patients. It can ensue when there is considerable pain or other complications: constriction of the bile duct or duodenum, pancreatic duct, pseudo cysts, pancreatic stones, blood vessels etc. There are different ways of operating while at the same time preserving the duodenum, depending on the initial situation.
Summing up, we can say that chronic pancreatitis is a grave illness, which is often belatedly diagnosed. As long as there is no acute deterioration, then yearly check-ups (ultrasound, laboratory tests) can be recommended. Acute bursts regularly demand stationary treatment.
Joachim Horcher